Monday on FNC’s “Tucker Carlson Tonight,” host Tucker Carlson laid out some examples of the unintended consequences of some pharmaceuticals to warn against the country’s dependency on drugs to cure every ailment.
The FNC host said those unintended consequences were disrupting human behavior and potentially causing problems for society.
CARLSON: We talk about it every night, multiple disasters all at once, but if you had to isolate one single tragedy that’s produced the highest casualty rate in the United States, it will probably have to be the opioid crisis.
Over the past 25 years, opioids have destroyed entire regions of the country, mostly rural areas, places populated by the people who built and fed this country for generations.
Hundreds of thousands of them have died from opioid, and they’re still dying, more than 100,000 drug ODs just last year, mostly from fentanyl.
Fentanyl is imported from China and smuggled through Mexico. If you live here, you probably know someone who’s died from fentanyl, probably someone’s child.
What you may have forgotten in the face of all this sadness is that the opioid epidemic was not organic. It didn’t just happen one day because people in sparsely populated zip codes in Kentucky and Vermont and West Virginia suddenly felt sad and started taking dangerous drugs. No.
This particular disaster was created by drug companies. That’s true.
Purdue Pharma kicked it off. They did so by aggressively marketing a narcotic called OxyContin. They sold it to doctors and doctors sold it to their patients on the false claim it was non-addictive. It was very addictive.
What happened next? Well, drive through upstate New York sometime. You can see the human carnage.
Ultimately, Purdue Pharma faced a barrage of lawsuits and then criminal charges. In the end, however, not a single executive from that or any other drug company ever went to jail. So, no one was ever really punished for all those deaths, hundreds of thousands of deaths.
Well, for a brief moment, it seemed possible that somebody would be punished.
No one remembers this, but during the Democratic primaries in 2019, Kamala Harris, of all people, described pharma executives as “nothing more than some high-level dope dealers” who “should be held accountable.”
Then a few months later, she went further than that. Harris suggested the drug companies were so evil they might produce a COVID vaccine that wound up hurting people. “If Donald Trump tells us we should take it, I’m not taking it,” Harris said. And then other Democrats, including Andrew Cuomo, then the Governor of New York, said the very same thing, but here’s the amazing part, the second Joe Biden took office, talk like that stopped immediately. Never has a tune changed faster.
Kamala Harris, who just months before had called drug companies dope dealers, suddenly sounded like the chief marketing officer at Pfizer. At one point, Harris announced that volunteers would go “door to door” to promote Pfizer’s products.
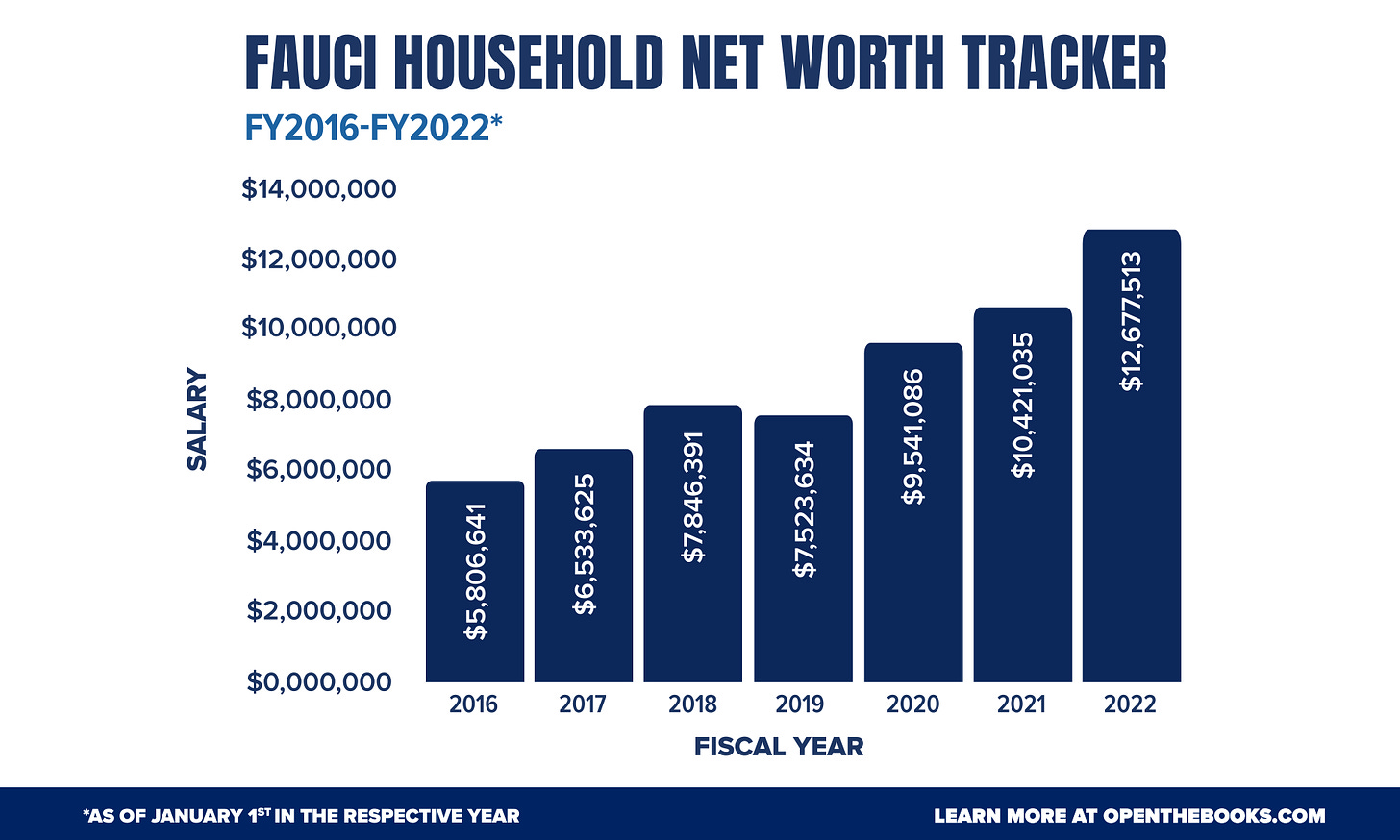
Never in our history have Federal officials touted a publicly held company more aggressively than the Biden administration touted Pfizer, and as a result, Pfizer’s stock price exploded. Its executives made billions.
Gone was any suggestion that the drug companies might be capable of doing anything wrong, ever.
Instead, the media and the Biden administration lauded pharma executives as moral heroes. And some of their products are lifesaving, that is true, but the bigger truth we are now learning is more complicated than that.
In just the past few weeks, serious, very serious questions have emerged about some of the most widely prescribed drugs in America, very much including the COVID vaccines.
But we want to begin tonight with what in any normal period would be front- page news around the world. It turns out the entire premise behind the most commonly prescribed antidepressant drugs appears to be completely wrong.
These drugs are known as SSRIs. They’re ubiquitous.
Between 1991 and 2018, total SSRI prescriptions in the US rose by more than 3,000 percent. The number of prescriptions for the most common SSRIs hit 224 million last year — 224 million prescriptions in a country of 330 million people.
In other words, you know, dozens of people who are taking SSRIs. You may be taking them right now. And yet for decades there have been strong indications that there is a problem with these drugs and the most obvious is this.
Antidepressants are supposed to cure depression. That’s why they’re prescribed. And yet, over the same period that SSRI prescriptions have risen 3,000 percent, the suicide rate, may be the most reliable indicator of all of depression has not fallen in the United States. In fact, the suicide rate has jumped by 35 percent. That’s a huge increase. That’s a lot of dead people.
Now, drug makers admit that their products may be part of the reason for the increase in suicide. The makers of Prozac, for example, can see that young people who take that drug have an increased risk of suicide compared to those who took a placebo.
Think about that for a second. A drug that’s supposed to make you less sad may make it more likely that you will kill yourself. How is that allowed?
Well, it’s been allowed because virtually no one has said a word about it. One person who did say something about it a long time ago was the actor, Tom Cruise, all the way back in 2005. He had a very famous appearance on “The Today Show.” You may remember it. Here it is.
(BEGIN VIDEO CLIP)
TOM CRUISE, ACTOR: Here we are today where I talk out against drugs and psychiatric abuses of electric shocking people, okay, against their will, of drugging children with them not knowing the effects of these drugs.
Do you know what Adderall is? Do you know Ritalin? Do you know now that Ritalin is a street drug? Do you understand that?
MATT LAUER, THEN NBC NEWS HOST: Aren’t there examples and might not Brooke Shields be an example of someone who benefited from one of those drugs?
CRUISE: All it does is mask the problem, man, and if you understand the history of it, it masks the problem. That’s what it does. That’s all it does.
You’re not getting to the reason why. There is no such thing as a chemical imbalance. Drugs aren’t the answer that — these drugs are very dangerous. They’re mind-altering antipsychotic drugs and there are ways of doing it without that, so that we don’t end up in a brave new world.
(END VIDEO CLIP)
CARLSON: So, Cruise said a few things. One, maybe you shouldn’t trust the pharma companies and just hand your children whatever they’re producing and hope for the best. Two, there is no such thing as a chemical imbalance in your brain that causes depression, he said that; and three, these drugs mask the real problems. You’re suffering for a real reason the drugs can’t fix.
Provocative statements. How did the country respond to this?
Well, everyone in the media agreed: “Tom Cruise is crazy. He’s in a cult. Shut up.” A lot of people thought that. We may even have thought that, but then more information kept coming out that made Tom Cruise look a little less crazy.
In 2015, researchers from the scientific journal BMJ found that, “Some birth defects occur two to 3.5 times more frequently” a lot more frequently, “among the infants of women treated with (SSRIs) early in pregnancy.” Well, that’s a huge problem — ignored.
In the same journal in 2020, researchers found that “Post-SSRI sexual dysfunction is under-recognized and can be debilitating both psychologically and physically.” Well, that’s kind of a problem, too. If it steals your sex drive, maybe it’s stealing your soul. No, ignore it. Only cult members care.
Then last year, researchers in Sweden found that: “There may be an increased hazard of violent crime during SSRI medication in a small group of patients. It may exist across age groups and throughout treatment periods and it possibly persists for up to 12 weeks after treatment discontinuation.”
So, even after you stop taking the drugs, you may be impotent, infertile, violent, but at least the drugs cure the chemical imbalance in your brain that causes your depression. That was the selling point.
What a great piece of marketing. You’ve got a chemical imbalance in your brain. You need these drugs, and so hundreds of millions of prescriptions every year for these drugs.
Well, in what seemed like news to us, last week we learned that actually SSRIs don’t cure a chemical imbalance in your brain.
So, the acronym SSRI stands for Selective Serotonin Reuptake Inhibitor. The theory was, has been for 30 years, that depressed people have an imbalance of serotonin in their brains. They have a chemical imbalance.
If you give them more serotonin, then they become less depressed and happy. They’re less likely to kill themselves. Right. But it turns out that serotonin deficiencies are not the reason people get depressed. That’s not just a guess, it is now officially science.
This new finding comes from University College London. It just completed a long and huge study on the relationship between depression and serotonin. It was published in the journal, “Molecular Psychiatry.”
Here is what the lead author of that study, Joanna Moncrieff, said about the findings, “I think we can safely say, after a vast amount of research conducted over several decades, there is no convincing evidence that depression is caused by serotonin abnormalities, particularly by lower levels or reduced activity of serotonin.”
What? That was the whole premise of the drug, which virtually the entire American population was taking on their doctor’s advice, and by the way, the drug companies made billions off those drugs.
So, first we were told that SSRIs would save lives. Now, we learn they don’t actually work as intended. In fact, the whole idea behind the drug was completely wrong. And yet, and here is the best part, people are ignoring this news and the drugs are still being prescribed.
How can that happen in a country based on science? Well, as it turns out, and this is the real point, that happens all the time.
On this channel just the other day, Tony Fauci, no less than Tony Fauci, admitted in public that actually we have no idea what effect the COVID vaccines might have on women’s fertility, on their menstrual cycles. Wait a second. Remember when suggesting that could get you bounced off of Twitter and Facebook as a conspiracy theorist? Well, it turns out it’s true. Here’s Tony Fauci.
(BEGIN VIDEO CLIP)
BRET BAIER, FOX NEWS CHANNEL CHIEF POLITICAL ANCHOR: There’s been a number of studies. “New York Times” just did one about menstruating cycles and how that is affected by vaccines.
DR. ANTHONY FAUCI, DIRECTOR, NATIONAL INSTITUTE OF ALLERGY AND INFECTIOUS DISEASES: Yes, though — well, the menstrual thing is something that seems to be quite transient and temporary. That’s the point. That’s one of the points. We need to study it more.
(END VIDEO CLIP)
CARLSON: Oh, we need to study it more. We need to study more. It’s just like human fertility, reproducing the species, the most important event in most people’s lives. We need to study it more. Oh, but it’s too late. We just forced millions of women to take that drug. Sorry.
So how did they release a vaccine and then make it mandatory when they didn’t understand the long-term effects of the drug? That’s a very good question.
Here’s Deborah Birx. She is the former White House COVID response director again on FOX News.
(BEGIN VIDEO CLIP)
DR. DEBORAH BIRX, FORMER WHITE HOUSE CORONAVIRUS RESPONSE COORDINATOR: I knew these vaccines were not going to protect against infection and I think we overplayed the vaccines and it made people then worry that it’s not going to protect against severe disease and hospitalization. It will, but let’s be very clear. Fifty percent of the people who died from the omicron surge were older, vaccinated.
(END VIDEO CLIP)
CARLSON: What? Stop the presses, “I knew these vaccines were not going to protect against infection.” Really, Deborah Birx? But somehow you forgot to mention that as people were being fired from their jobs for not taking this on the premise that if they took it, they would never be infected? When do you get criminally charged? Soon, we hope.
And then there’s the effect of the COVID vaccines on the elderly, the population most at risk. According to “The Lancet,” no less than, vaccinated people around Joe Biden’s age are 80 percent more likely to become sick after taking the COVID shot as compared to unvaccinated people.
Wait. What? Eighty percent more likely to become sick after taking the shot that was supposed to prevent them from getting sick? How is this not the banner headline? It’s being ignored.
Well, as one scientist wrote in the “Journal of Virology,” “The study showed that immune function among vaccinated individuals eight months after the administration of two doses of the COVID-19 vaccine was lower than that among the unvaccinated individuals.”
So, it’s not just that your natural antibodies were more powerful than the vaccine. We’ve known that for a long time, though they lied about it. It turns out the vaccine appears to depress your immune system. This has massive implications, not just for COVID. There are all kinds of horrible diseases you can get with a suppressed immune system.
“The Journal of Food and Chemical Toxicology” found the same thing: “Vaccination induces a profound impairment in type one interferon signaling, which has diverse adverse consequences to human health.”
What the hell. And yet these people are on TV blithely admitting, “Oh, well, we should do more study on that,” after we forced it on the entire American population, on billions of people globally.
And this might explain how Joe Biden got COVID after getting every available shot and telling us just a year ago that vaccines conferred total immunity.
(BEGIN VIDEO CLIP)
JOE BIDEN (D), PRESIDENT OF THE UNITED STATES, JULY 21, 2021: The various shots that people are getting now, cover that. You’re okay….You’re not going to get COVID if you had these vaccinations.
BIDEN, JULY 22, 2022: Hey, folks, guess you heard. This morning I tested positive for COVID, but I’ve been double vaccinated, double boosted.
(END VIDEO CLIP)
CARLSON: So, one of the response to this is great sadness, of course, because even people who didn’t vote for Joe Biden believed his administration when they said this because they were acting in the name of science. People were afraid of COVID. In some cases, with great justification. Some people were at risk of dying from COVID and they reached out and accepted this drug on the promise told to them repeatedly that it would save them.
And now you have Deborah Birx says, “I knew it didn’t really work.”
So, the question is, why is no one being held accountable? Why is the party that promised to hold Big Pharma accountable ignoring this? They’re not saying a single word about any of these lies from the pharmaceutical industry, which is making billions and there’s more. There’s more.
It turns out that Alzheimer’s drugs, the most widely prescribed Alzheimer’s drugs, don’t actually treat Alzheimer’s. You know, does Viagra — that appears to work because in 2022, nothing is too weird to be true, but that’s not what they’re prescribing.
In 2014, in the journal “Alzheimer’s and Dementia,” researcher Jeffrey Cummings found a 99 percent failure rate of Alzheimer’s treatments in the pipeline for production, but he suggested that further treatments would be more successful.
Well, how does that work? Because the new medications, Cummings wrote, would effectively target the proteins that form so-called sticky plaques in the brains of people who suffer from Alzheimer’s.
Just like a lack of serotonin was thought to cause depression, sticky plaques in the brain were thought to cause Alzheimer’s. If you’re interested in the subject, you’ve definitely read that.
So, these new drugs came out. They’re very expensive. Did they work? No, they failed.
Two new Alzheimer’s drugs, one from the drug company Genentech, the huge biotech firm, Genentech, the other from Biogen were supposed to target sticky plaques and they did, but here’s what they didn’t do, fix Alzheimer’s. They did nothing to affect Alzheimer’s.
Incidentally, the FDA approved Biogen’s drug despite a ten-zero vote from the FDA’s own advisory committee to reject it. What?
So, it turns out that the assumption about sticky plaque causing Alzheimer’s is likely wrong, and the people running our public health establishment knew what was wrong, but ignored the fact it was wrong. And again, no one’s being held accountable. The entire population, trusts the science.
If you want to make people distrust the science and go to the witch doctor rather than the pediatrician to treat their kid’s flu, this is how you act. You lie and then you never admit it, apologize, or hold the liars accountable.
So, the claim that sticky plaques caused Alzheimer’s originated in a 2006 paper in the journal, “Nature,” and it was written by neuroscience professor Sylvain Lesne.
Recently, a Vanderbilt University neuroscientist called Matthew Schrag took a closer look at that 2006 paper, so did “Science” Magazine. What did they find? We’re quoting, “Shockingly blatant, fraudulent data,” according to Donna Wilcock, who works on Alzheimer’s at the University of Kentucky.
Elisabeth Bik, a molecular biologist reported that “Data might have been changed to fit a better hypothesis.”
Holy smokes. So, how did the NIH, which is working with your money on your behalf to keep the nation healthy, how did they respond to this? Well, they awarded that same scientist a new grant to study Alzheimer’s and the Democratic Party, Pharma’s new best friends. Haven’t said a word about it. Instead, they’re finding new ways to send your cash to their donors. Here’s a new trans admiral.
(BEGIN VIDEO CLIP)
ADM. RACHEL LEVINE, ASSISTANT SECRETARY FOR HEALTH: So, we really want to base our treatment and to affirm and to support and empower these youth not to limit their participation in activities to sports and even limit their ability to get gender affirmation treatment in their state.
(END VIDEO CLIP)
CARLSON: So, whatever you think of the trans question, kids struggling with questions about gender identity, notice the first thing that person says, the salient point that person makes is that a drug can fix it. Really? More drugs.
So the same people who had no clue what SSRIs did and then pushed them for decades, the same people who are making toddlers take the COVID shot despite the obvious risks and no data whatsoever to support giving it to toddlers, the same people who fast-tracked useless Alzheimer’s drugs to the elderly, are now telling you that kids with gender identity disorders must have more drugs. And the administration that promised to hold Big Pharma accountable cheers them on.
Maybe at this point, we should acknowledge that drugs are not the answer to every human problem. People are more than just a collection of chemicals that could be manipulated to produce a desired result.
They’re human beings. They have souls. If they’re sad or sick or alienated from other people, it’s just possible that Pfizer is not the solution.